Engineering Vision Researchers are working to cure blindness with
microchips and electrodes. Stephanie Pappas takes
a close look. Illustrated by Noel Pugh and
Lauren Hennessy. 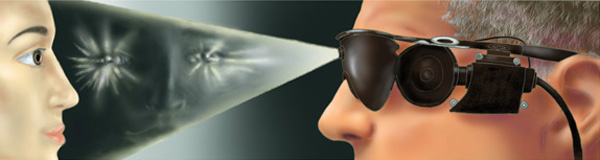
Illustration:
Noel Pugh
Linda
Moorfoot couldn't understand why her vision was failing. At 21,
unable to see objects right in front of her, she visited an
ophthalmologist. The diagnosis was grim: The light-sensitive cells
in her eyes were dying, snuffed out by retinitis pigmentosa, a rare
and incurable genetic disorder. The doctor predicted Moorfoot would
be blind by the time she was 30. Moorfoot
held out longer than her doctor expected. She spent the next three
decades raising three daughters and learning the corners and edges
of her Long Beach home by heart. But by age 52, the darkness closed
in. Eight years later, in May 2004, her
doctor mentioned a new clinical trial at the University of Southern
California. Researchers were developing a device to restore vision,
he said, and were looking for retinitis pigmentosa patients like
her. Intrigued, she went across town for testing. Months later,
she learned she was eligible for a cutting-edge implant to replace
her ruined rods and cones. Moorfoot was
used to blindnessNever used a cane and never had a dog, just went
about my business and doing all the things I ever did except drive,
she saysand was nervous at the prospect of surgery. She had no
guarantee her sight would return. It wasn't until she was playing
with her five-year-old grandson one day that she made her decision.
He said, 'Well, Grandma, if you do this surgery
will you be able to see me?' she says. She remembers thinking that
even if her vision didn't improve, she could help pioneer a cure
for future generations. A few months after
that, Moorfoot became one of the first people to test the Argus 16,
an artificial retina that lets her see lines, shadows, and the
shapes of her grandchildren running across a soccer field. The retinal replacement, a tiny implant that
translates light into neural signals, was twenty years in the making.
With funding from the National Science Foundation and the U.S. Department of Energy, a team of researchers
at 11 institutions brought the device to clinical trials in 2002.
Since then, they have reintroduced sight to dozens of patients in
America, Europe, and Mexico. Now, the team is working to create a
higher-resolution retinal prosthesis that will allow patients to
see faces and even read large print. From
science fiction to fact The project began
with USC ophthalmologist Mark
Humayun, who grew up watching his grandmother lose her vision
to diabetes. I saw the problems of vision
loss early and on a very personal level, he says. Even then, I
made a commitment to being an eye doctor and doing what I could to
alleviate the suffering and problems that blindness can bring.
Years later, with treatments for degenerative
retinal diseases still out of reach, Humayun approached Wentai Liu,
an electrical engineer at North Carolina State University, and asked
him to help build an electrical system to replace the retina.
It sounds like a science fiction story, says
Liu, from his office overlooking the redwood trees at UC Santa Cruz,
where he's worked since 2003. His walls are lined with awards and
honors, including a Dutch textbook propped up on two nails. Inside
is a picture of him holding the microchip that drives the artificial
retina. When Liu joined the project in 1988,
the team didn't know if stimulating the remaining cells in the eye
of a retinitis pigmentosa patient was possible. But circuits are
one of Liu's passions, and he jumped at the chance to design the
mechanism. Liu says he has no financial stake in the artificial
retina, which will be sold through the Sylmar, Calif.-based company
Second Sight. And though he loves the work, he sometimes chafes
under the hush-hush requirements of for-profit engineering. I'm an academic, he says. I prefer to have free
exchange of information. Liu does his
engineering in a cramped fourth-floor lab filled with computers
that hum and beep and heat the air. Spools and tangles of colorful
wire litter a table near the door. He
eagerly shows off some of his team's latest projects:
a wireless EEG cap, a microstimulator for the eyelid, a navy blue
baseball cap with Wentai Liu embroidered in script and EEG-monitoring
electrodes lining the band. You can wear it while you're driving,
he explains, and if you begin to fall asleep, it will call your
cell phone and wake you up. But creating
a circuit that works inside a living eyeball has been Liu's
longest-running challenge. Engineering in the
eye In a healthy eye, the lens focuses light
onto the retina, a half-millimeter-thick tangle of light-sensitive
cells coating the back of the eyeball. Here, the eye begins to
organize light, sorting and translating wavelengths into neural
pulses. The pulses shoot down the optic
nerve to the brain's visual cortex, where densely packed neurons
synthesize information about color, orientation, and depth into
faces, mountain vistas, or words on a page. Any
break in this chain can lead to blindness, but degenerative retinal
disorders are untreatable. Vision researchers are testing new drugs
and gene-therapy techniques but, Humayun points out, blindness is
winning the race. His goal is not to slow or stop the progress of
retinitis pigmentosa and related
disorders, but to reverse the effects. Although
retinitis pigmentosa damages light-sensitive rods and cones, it
generally spares the information-carrying cells layered over the
photoreceptors. The artificial retina taps into these with a tiny
array of electrodes. Patients wear a video camera on a pair of
eyeglasses. As they move their heads to scan over objects, the
camera wirelessly transmits images to a receiver, which rests under
the skin either behind the ear or by the eye. From there, the
signal travels to the array, which fires its own electric pulses
down the optic nerve. 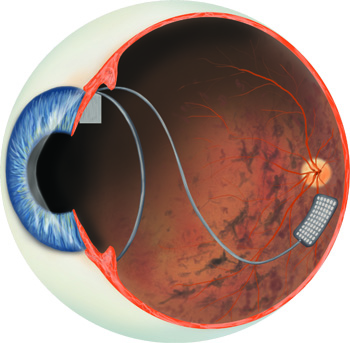 | Illustration: Lauren Hennessy |
Humayun's team has tested the
artificial retina only on patients with retinitis pigmentosa, which
affects about 100,000 Americans. But the team also hopes to target
age-related macular
degenerationone of the leading causes of blindness in the United
States, affecting more than 1.7 million people. To
tackle a project this big, the researchers had to think small. The
implant must fit into a space the size of a ping-pong balla wet,
salty, corrosive ping-pong ball. The electrodes must stick to the
fragile fabric of the inner eye. And to reduce the risk of infection,
the engineers can't use wires to transmit either data or power.
People always ask, hey, if an engineer can
design a cell phone and receive information wirelessly, why is it
difficult to transmit the camera data and receive video data to the
eye? Liu says, pulling his cell phone out of his pocket. The
reason is, the engineers that designed this onehe waves the phone
aroundthey don't have any limitations on the size. When Moorfoot received her implant in 2004, she
was one of six people testing the Argus 16, a model that already
seems clunky. It has just 16 electrodes, and the inch-long transceiver
that relays camera data and power to the array was scavenged from
larger cochlear implants designed for the inner ear. Still, the device satisfied some of the team's
goals. Specially developed hermetic packaging kept the eyeball's
fluids out of the circuits. The electrode array, tacked to the eye
with a staple the width of a human hair, stayed put. Most importantly,
the device worked: At first, Moorfoot saw specks of light, like an
incomplete connect-the-dots puzzle. But as she practiced with the
video glasses, learning how the world matched up to this new version
of vision, the dots crystallized into lines, cueing her in to edges
and corners. And Liu's circuits kept the
whole thing running. The circuits transfer
energy wirelessly from battery pack to implant using two coils to
create a magnetic field, which is then converted to electricity.
The system is also what Liu calls intelligent. When the user looks
at something bright, the circuits sense the need for extra power.
If one patient wears her glasses farther out on her nose than
another, the system can sense that too, ramping up the signals from
the camera to the receiver. And no, you
can't leave the glasses at a neighbor's house and use them as a
spy-cam; the video signal travels only a few centimeters. Still,
the device has its moments. Moorfoot once forgot to switch the
camera off while on a Disneyland rollercoaster. She squeezed her
eyes shut on the ride, but to no avail. The camera kept flashing
dizzying light right to her optic nerve. Seeing
red (tape) After the success of Argus 16,
the team scaled the power up and the size down. The Argus II, which
began clinical trials in the United States in 2006, has 60 electrodes
and a transceiver the size of an aspirin. As
the electronics gets smaller and the amount of data to transfer
grows, Liu has had to develop more powerful chips. More power means
more heat. That's fine for a cell phone, but it's not so great for
the human body. We cannot allow the temperature to rise more than
one degree Celsius, Liu says, because it would damage the eye.
Besides abiding by National Institute of Standards
and Technology standards on heat, Liu and his team also must answer
to the Federal Communications Commission, which regulates radio
frequency. Those regulations are one of the
toughest challenges, says Moo Sung Chae, a graduate student who has
worked with Liu for four years. The team once had to redesign a
microchip when the chip's frequency interfered with AM radio.
To shepherd the project through yet another
layer of regulationsstringent U.S. Food and Drug Administration
protocols for clinical trialsHumayun's group partnered with Second
Sight in 1998. The decision to go commercial catapulted the team
over similar efforts around the country, including a Veterans
Affairs-funded collaboration in Boston. It's
tough to do it with fewer resources, says Shawn Kelley, a researcher
for the Boston group. With Second Sight
behind them, Humayun's group has met success in clinical trials.
Four of the six original Argus 16 patients still use their retinal
implants (the other two have since died of unrelated causes). And
nine of the ten patients implanted with the 60-electrode Argus II
are still using it. But the device isn't
perfect yet, cautions Brian Mech, vice president of business
development at Second Sight, noting that the clarity of sight varies
from patient to patient. Researchers are still teasing out why,
but the original condition of the retina and the type of genetic
mutation causing the retinitis pigmentosa may make a difference.
Other possible factors are the degree to which each individual's
brain can "re-wire" itself, and the recipient's enthusiasm
for the training. Starry-eyed One enthusiastic recipient is Dean Lloyd, a
68-year-old Palo Alto lawyer who developed retinitis pigmentosa
during medical school. He had to drop out when he could no longer
see through the microscope, but he went on to work as a biochemist
and then as a software engineer before switching to law.  | Photo: Stephanie Pappas | Retinal implant recipient Dean Lloyd wears his
video glasses outside his law offices in Palo Alto, California.
| | Lloyd
found out about the Argus II trials through his daughter, Lisa, who
works for Foundation Fighting Blindness in Northern California.
The organization put up seed money for initial development of the
device. Lloyd didn't hesitate to apply, and on July 10, 2007, he
became the seventh person in the United States implanted with the
Argus II. The path hasn't been completely
smooth. Lloyd had a second surgery to re-tack the electrode patch
because not all of the electrodes were resting flush against his
retina. And because some of the outermost electrodes need more
power than the FDA has approved, he isn't using the full array of
60 dots. Lloyd's experience provides some
insight into the differences between the Argus 16 and the Argus II.
At various points, he's had as few as nine and as many as 52
electrodes firing. Boundaries get sharper as the number of electrodes
go up, he says, using the example of a statue he saw the first time
he walked outside wearing video glasses. With nine electrodes
active, he knew something was there, but couldn't tell what. Now,
he says, the borders are crisper, though not crisp enough to discern
the statue's face. The world through the
Argus might look a bit like opening a black-and-white picture on
Photoshop, upping the contrast, lowering the brightness, and throwing
in some pixellation. Sharply contrasting areas remain, but their
resolution isn't high. Moorfoot describes lines lighting up as she
scans over things. Lloyd can see the reflection of moisture in
people's eyes, like a cat under a bed where you shine a flashlight.
He sees shapes in flashes of light: cars coming by, his daughter's
hands. People come up to me and ask, What
do I look like? he says. His response? Oh, you are a star, in
fact you're many of them. Lloyd still travels
to San Francisco for visual training. He's working on spatial
recognitionfiguring out how the lines and borders he sees relate
to one another. It's a learning process he's introduced into his
daily life, as well. When he sees a flash of light from his implant,
he makes a point to explore the object that triggered the electrodes.
He's taught himself to recognize doorframes and the curb along his
favorite walking path. I'm not gonna throw
out my hickory [walking] stick, Lloyd says. It's vision that's
useful, but in a different way. Like Moorfoot,
Lloyd says he wanted to be a part of the study for the sake of
future generations. His daughter Lisa Lloyd has a mosaic case of
retinitis pigmentosasome of her retinal cells are affected, while
others are healthy. Definitely progress
is happening in this area, she says. It's really exciting for
people like me who are slowly going blind. You just think, oh, is
there anything out there for me, am I going to be okay? Others strike a cautious tone. Frank Welte,
director of advocacy and government for the California Council of
the Blind, calls the research interesting, but warns it could be
decades before science accurately mimics human sight. If there were something developed for my situation,
I might be interested in it, says Welte, who has retinopathy of
prematurity, a disorder that strikes preterm babies and made him
blind at birth. But I'm not putting my life on hold waiting.
Second Sight expects the Argus II to be its
first commercially available device, hitting the United States
market in 2010. Mech said the company hasn't set a price, but
suggested the Argus II would cost more than a cochlear implant.
That could put the price between $60,000 and $100,000. Meanwhile,
he hopes to start clinical trials in 2011 for a third generation
of the device with more than 200 electrodes. Looking to the future The
team's grand aim is to develop a device with more than 1,000
electrodes that can fit inside the eye, camera and all. The design
would allow users to take advantage of their natural eye movements
instead of having to turn their heads to scan over objects.
The scientists also are trying to determine how
many more electrodes they will need for patients to recognize faces
and read large print. After all, 1,000 still falls far short of
the millions of light receptors in a healthy retina. Simulations
suggest that better acuity is possible, says Liu, but until the
1,000-electrode device is tested in humans, there's no way to be
sure. And no one seems quite confident that the camera-in-the-eye
design is feasible anytime soon. Right
now, the next-generation microchip waits in Liu's lab. Under the
microscope, the chip is a sleek gold grid with spaces for 256
electrodes. It can easily be scaled up to 1,024 electrodes, Liu
says. But with that will come challenges for power and data
transmission. For Liu, it's a project
worth pursuing. He sees bioengineering as the future, a way to
help the less fortunate and solve societal problems. Lloyd and Moorfoot look forward to that future as
well, and hope they have been a part of making it real. In the
meantime, they and others like them will keep navigating a world
painted with lights and lines and stars. I
just have fun with it, Moorfoot says. I'm waiting for them to
improve it and do something better, like when they get the 250 and
the 1,000. If I'm not too old, I'll do it again. Editor's note: In August 2009,
R&D magazine awarded its prestigious R&D 100 Award to the artificial retina project,
recognizing it as one of the nation's most innovative ideas in
research and engineering. Story 2009
by Stephanie Pappas. For reproduction requests, contact the Science Communication Program
office. Top
Biographies  Stephanie Pappas Stephanie Pappas
B.A.
(psychology) University of South Carolina
Internship: Stanford
Medical Center news office
I made
my way to California incrementally, hop-skipping from the sand hills
of South Carolina to the thin-aired Rockies, and finally alighting
in the redwood forests of Santa Cruz. My
journey into science writing has been much the same. I rebelled
against crunching numbers in a neuroscience lab; instead, I spent
valuable data-gathering time listening to the life stories of our
study participants. Concluding that I was more interested in people
than in science, I landed in education. I taught children with
autism, but I found that I wanted to know how their brains worked.
My mistake was in believing that science and people occupy separate
spheres. Science writing is my way of exploring both. And whether
I find myself in South Carolina or Santa Cruz, I know there will
be stories to tell. . . . . . . . .
. . . . . . . . . . . . . . . . . . . . . .
. . . . . . . . . . . . . . . . . . . . .
 Noel Pugh Noel Pugh
B.F.A.
(painting) San Francisco Art Institute
Internship: Illustrating
a field guide of native bees for researcher Gretchen LeBuhn, San
Francisco State University
Whether
pondering the birth of a cloud while lying in the grass, or studying
the proboscis of a bee while looking through a magnifying glass,
my heart and mind are forever turned to illustrating this world,
which is full of wonder. . . . . . .
. . . . . . . . . . . . . . . . . . . . . .
. . . . . . . . . . . . . . . . . . . . . .
. 
Lauren Q. Hennessy
B.A. (fine art) UC Santa Cruz
Internship:
UC Davis Tahoe Environmental Research Center, Tahoe City, CA
When choosing a direction to go in college, I
was torn between my passions for drawing and science. I quickly
fell in love with the printmaking department at UCSC and decided
to pursue a degree in studio art. During one of my first art
courses, I was encouraged by the professor to look into the Science
Illustration Program. I then realized I didn't have to make a clear
distinction between art and science and could have a career combining
them. To see more examples of my work, see my web
site.
Top | 
