Scientists try to discover nature's chemical recipe
for protecting young women from breast cancer

Imagine if women could practically assure themselves they would not become one of the one-in-eight women in this country to suffer from breast cancer. They can, but it's not by buying and taking a pill. The cancer-fighting secret is natural and it's free -- but comes at quite a cost to modern women. The protective mystery-molecule appears during a woman's first pregnancy. The unknown chemical, however, seems to be highly effective only if a woman gives birth before the age of 20.
Despite the benefits, it's not likely physicians will be asked to prescribe pregnancy to teen-agers as a prophylactic against breast cancer. Teen pregnancy is a social taboo, and career-minded women, with the help of technology, are safely delaying pregnancy. But scientists think they are close to finding an acceptable alternative that will offer the same protective effects as early pregnancy.
For thirty years, researchers tried to find out how lactogenic (milk-producing) hormones, like prolactin, suppressed breast cancer. Now scientists at the University of California at Santa Cruz say the answer is less obvious, involving more than the pregnancy hormones investigated to date. Their new data suggests a complex dance of several chemical messengers, led by a hormone that plays a part in many bodily transformation, not just pregnancy -- growth hormone (GH). They are now testing their theory in hopes of one day mimicking the protective result of pregnancy without actual gestation and childbirth.
Relative Risk
In fact, it's been 30 years since epidemiologists alerted scientists to a surprising trend. They observed that nuns had a significantly higher rate of breast cancer than the rest of the population. Scientists following up these studies soon focused on the potential role of pregnancy in protecting women against breast cancer. They found a woman's age at her first full-term pregnancy predicted her risk of getting breast cancer. Women who gave birth before the age of 20 were 50 percent less likely to develop breast cancer than women who had never given birth. The protective effect of pregnancy (PEP), however, decreased as a woman aged. Her risk actually surpassed that of a childless woman if she gave birth to her first child after the age of 34.
Most researchers suspected the pituitary hormone prolactin and the ovarian steroids estrogen and progesterone caused the PEP because their presence in blood rises dramatically during pregnancy and are important to breast development. But strong evidence is still scarce, even after decades of research.
UCSC professor of endocrinology Frank Talamantes is credited by his colleagues with bringing a unique perspective to breast cancer research. "Most people studying breast cancer were not endocrinologists," says Talamantes. Cancer researchers, trained to look to genes or inherent properties of cells, often overlooked the chemical messengers that travel between them. "People had become narrow minded," Talamantes says.
Talamantes possesses an intimate knowledge of all pregnancy-related hormones. He and his colleagues previously showed GH decreases significantly in the blood of pregnant rats. "Very little growth hormone is free during pregnancy," says Talamantes. The cause and potential function of the decrease remain unknown. But, scientists report a substance known as a binding protein attaches to the hormone, making GH levels fall in the blood.
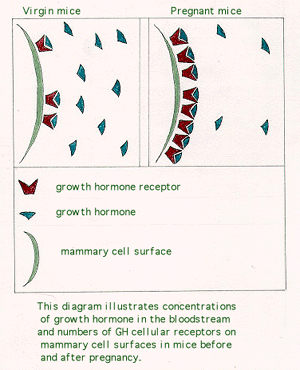
Receptors, proteins with individual shapes on the surface of cells, normally serve as locks to a cell. Normally, they are opened by a specific hormone or other protein. When bound, GH is unable to open the lock and enter the cell. Bound GH also can't be detected in the blood.
The decrease in GH seen in rats is postulated for women, as well. Rats, therefore, are used as the model system for human pregnancy. And virgin rats, when exposed to carcinogens, develop breast cancer at a higher rate than previously pregnant rats, as is the case with humans, Talamantes says.
Searching for Clues
But why implicate GH alone among the complex hormonal changes taking place during pregnancy? Just because GH happens to decrease doesn't mean its reduction in the blood is protecting women against breast cancer. But sometime during his training, Talamantes filed away a bit of data in his mind -- another natural experiment involving growth hormone. People afflicted with gigantism had something in common with nuns. They also had an increased rate of breast cancer. Gigantism is a result of having abnormally high levels of GH.
"He invigorated the field," says Dan Medina, professor at the Baylor College of Medicine in Houston. "The focus is now on a new mechanism."
Exposing Nature's Secret
That mechanism is proving to be a complex one. Levels of GH, it turns out, influence the activity of other pregnancy-related hormones. Talamantes and his colleagues measured levels of these hormones and their receptors in 1995. They reported lower levels of estrogen receptors (ER) and epidermal growth factor receptors (EGF-R) in previously pregnant rats compared to virgin animals. The hormones associated with these receptors, estrogen and epidermal growth factor (EGF), normally spring their respective locks, making breast cells grow, specialize and, in the case of EGF, divide.
Talamantes thinks EGF induces cell-division in mammary glands, the same role it plays in the liver. GH, he suggests, encourages the proliferation of these receptors in mammary glands. Reduced levels of GH in previously pregnant animals, in turn, means fewer receptors susceptible to lock-picking carcinogens that produce unchecked cell division, resulting in deadly tumors.
Talamantes and his colleagues are now trying to determine whether pregnancy alters the chemical surroundings of mammary cells through changing in the levels of GH or permanently alter the cells themselves after exposure to GH, causing them to develop tumors. In the lab's current approach to solving this problem, Gudmundur Thordarson, a senior scientist in Talamantes' laboratory, manipulates circulating levels of growth hormone and measures resultant levels of the receptors ER and EGF-R. Talamantes hypothesizes rats with less GH will produce fewer of these receptors.
The Big Picture
The clues Talamantes and Thordarson uncover promise to provide details about the hormonal basis of cancer, a disease whose mechanisms are poorly understood. But the clues won't yield a complete answer as to why such cancers occur, says Talamantes, because researchers know too little about the life cycle of even normal cells. "We don't know what makes normal cells divide," Talamantes says. "We've been putting the cart before the horse." Thordarson, however, remains optimistic. "Hopefully we can improve treatment for breast cancer patients," he says. "That's the whole idea."
Talamantes and Thordarson trust that their fellow scientists will focus on the hormonal basis of breast cancer and complement their own studies. Until now, the most celebrated advances in breast cancer research came from discoveries of the genetic causes of the disease. But many scientific and sociological steps separate the identification of genes and the use of gene therapy to treat the disease. Gene therapy enjoys a low success rate in part because it requires changing DNA. Also, the ethical issues raised by gene therapy have been hotly debated among both scientists and policy-makers. Gene therapy, in brief, is far from becoming a reality.
Hormone supplements, on the other hand, are already widely used with great success. Dwarfism, for example, is caused by a lack of growth hormone and can be partially treated with injections of the chemical.
Hormone supplements would seem to offer the ideal solution if Talamantes' hypotheses prove to be correct. "You can't ask every teenager to get pregnant," says Medina. "But you can find out what hormones are doing."